Broken blood vessels, also called “spider veins” or telangiectasia, are enlarged or dilated veins just below the surface of the skin that result in small, red lines spreading out into web-shaped form. Spider veins may develop anywhere on the body, but they are more common on the face and legs. Although broken vessels are harmless, they may become a nuisance if they make you self-conscious. However, broken blood vessels are typically treatable.
Broken blood vessels causes
Broken blood vessels tend to develop more frequently in some people than in others. In addition, spider veins can affect anyone at any age, even children.
The most common broken blood vessels causes include:
- Genetics. The reason for the tendency of telangiectasia to run in families is unknown. In addition, the individual risk of spider veins development increases with age.
- Exposure to the sun. Blood vessels may enlarge in response to excessive sun exposure. After a sunburn, the top layer of skin may peel off, temporarily exposing some blood vessels on your body.
- Pregnancy. During pregnancy, estrogen levels can increase, resulting in broken blood vessels. This type of spider vein usually goes away on its own after delivery.
- Injuries. A variety of injuries may result in bruising. Broken blood vessels may also be visible when you have bruises on your body.
- Changes in the weather. The hot weather causes blood vessels to dilate.
- Consumption of alcohol. Due to the enlargement of blood vessels caused by moderate or occasional alcohol consumption, your skin may flush. In addition, broken blood vessels are caused by heavy drinking or binge drinking.
- Pressure caused by sneezing or vomiting. When you sneeze or vomit violently, the blood vessels in your face can be ruptured due to intense pressure.
- Rosacea. It is a skin condition resulting in flushing and excessive redness. Moreover, in the case of erythematotelangiectatic rosacea (ETR), broken blood vessels may develop.
- Corticosteroids. Prolonged usage of topical or oral corticosteroids may lead to broken blood vessels.
- Chemical or environmental irritants.
Broken blood vessels symptoms
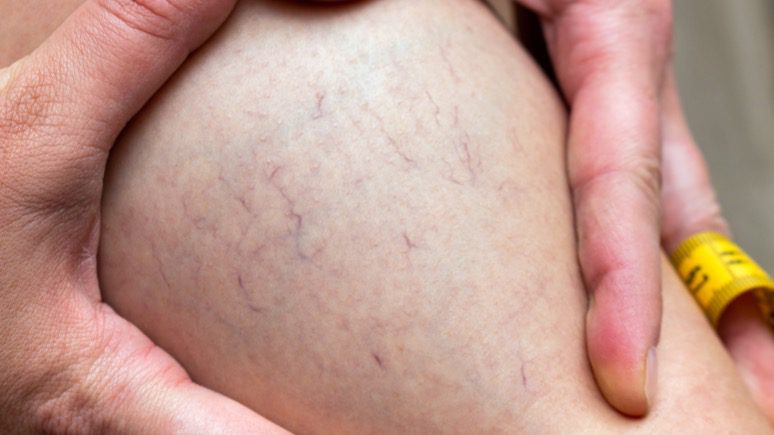
Broken blood vessels are fine, threadlike stripes. Usually red or pink, these lines become white under pressure. However, these tiny lines that form due to telangiectasia may become blue or purple with time. Broken blood vessels are typically 1 to 3 millimeters in width. Spider veins are usually harmless but may result in pain and itching.
Broken blood vessels commonly appear on the chin, nose, and cheeks, leading to facial redness. In addition, telangiectases often occur on the legs, arms, back, and chest. Many people refer to broken blood vessels on the legs as spider veins. Spider telangiectasia is characterized by a red, central feeding vessel and branches extending outward.
The best treatment for broken blood vessels
Even though telangiectasia has no cure, this condition can be managed. Your healthcare provider will prescribe you an appropriate treatment based on your symptoms, cause, and diagnostic tests.
Broken blood vessels resulting from rosacea or acne may be treated with oral or topical medications.
Patients with telangiectases may opt to have them removed, both for cosmetic reasons and because they may cause discomfort. To remove spider veins, the doctor may use sclerotherapy, laser therapy, or excision surgery.
- Laser therapy. The most straightforward method for treating telangiectasia and broken capillaries is laser therapy. The widened blood vessels can be sealed using laser ablation without much pain and with a short recovery time.
- Sclerotherapy. The standard treatment for broken blood vessels on the legs is sclerotherapy. In addition, larger veins respond best to sclerotherapy. This minimally invasive procedure involves injecting saltwater or the chemical solution into the affected vein. It will result in the hardening and disappearing of the veins. Sclerotherapy is effective in treating broken blood vessels, but it can take a long time.
- Excision surgery. Widened blood vessels can be removed with excision surgery, but this procedure has a prolonged recovery period and causes significant pain.
In order to prevent broken blood vessels and complement their treatment, you can also take the Khavinson peptide supplement called Vesugen. Vesugen contains peptide bioregulators of blood vessels isolated from plants. This supplement is designed to improve blood circulation and strengthen the cardiovascular system. However, it is not a medication. Instead, Vesugen is a supplement that complements the primary treatment.
Click here to read more about Vesugen.















Leave a Reply
You must be logged in to post a comment.