What is Spina Bifida?
Spina Bifida is a congenital disability with an incomplete closing of the backbone and tissue around the spinal cord. Spina Bifida is one of the most widely recognized congenital disabilities which impact the spinal cord. Spina Bifida starts in the womb when the tissues that overlap to frame the backbone do not close or develop properly. This causes an opening in the vertebrae, which encloses and surrounds the spinal cord. This happens within the first 30 days after inception—more often than not before the woman realizes that she is pregnant.
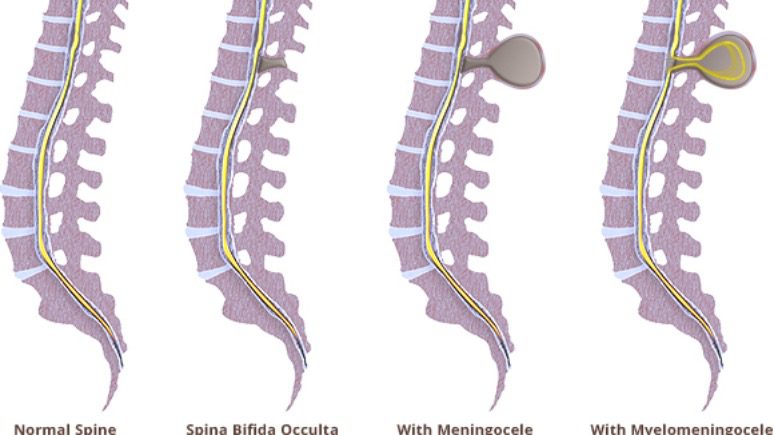
There are three types of Spina Bifida:
- Spina Bifida Occulta: Spina Bifida Occulta means “a hidden spot on the spine.” Spina Bifida Occulta is normally found inadvertently when the individual has an X-ray or MRI for some other reason. The pervasiveness of Occulta is not known, but unfortunately, it is the most widely recognized Spina Bifida cause.
- Meningocele: This is the least common type of Spina Bifida. The membrane that surrounds the spinal cord protrudes through the opening, causing a lump or sac on the back. This severe type of Sina Bifida can be surgically repaired with little to no nerve damage.
- Spina Bifida Cystica (Myelomeningocele): This is the most severe form of Spina Bifida. Spina Bifida Cystica, for the most part, includes neurological issues that can be intense or even fatal. A portion of the spinal cord and the nerves that surround it are protruding and are not covered by skin.
Surgery is a successful treatment for most children with Spina Bifida. Most newborns with an open spine or Myelomeningocele experience surgery within the initial 48 hours of life to close the deformity. In addition, anti-infection medicines are given to prevent infections of the uncovered spinal cord and nerves until the point that this defect can be corrected by surgery.
Prevalence
Spina Bifida affects approximately 1 out of every 2,500 newborns in the world. It is less common in African-Americans than in Hispanics and Caucasians in the United States. Spina Bifida occurs more often in children of parents who have the condition, but there is not a known genetic defect associated with the condition.
Spina Bifida causes
The precise Spina Bifida cause is not known. For instance, women who have had one child with Spina Bifida may not have another child with the illness. In addition, women who are overweight or who have diabetes are additionally more at risk to have a child with Spina Bifida.
Spina Bifida risks
Even though specialists and analysts do not know the exact Spina Bifida cause, they have recognized a couple of factors that increase Spina Bifida risks:
- Race: Spina Bifida is more typical among Caucasians and Hispanics.
- Gender: Females are impacted more frequently.
- Family history: Couples who have had one child with Spina Bifida have a somewhat higher possibility of having another child with a similar congenital disability. The Spina Bifida risks increase if two past children have been influenced by the condition.
- Folate insufficiency: A lack of folate in the diet is a theory on what causes Spina Bifida.
- A few medicines: Reactions to seizure prescriptions, for example, valproic acid (Depakene), appear to cause neural tube deformities when taken amid pregnancy by interfering with the body’s capacity to process folate and folic acid, so it increases the risk of Spina Bifida development in a child.
- Diabetes: Diabetes is another probable cause of Spina Bifida in women. Women with diabetes who do not control their glucose may have a higher risk of Spina Bifida development in their child.
Complications
The outcome of Spina Bifida depends on the severity of the condition. Some patients live completely independent lives, and others who have a severe injury to the spinal cord require life-long care. The infant mortality rate for Spina Bifida has improved with advancements in neonatal medicine.
Click here to read about the Symptoms.















Leave a Reply
You must be logged in to post a comment.